|   |
|   |
When generating invoices, AWARDS searches for any clients in the selected program billing group who have all of the client data required for billing, including: name, date of birth, gender, address, a diagnosis code, and an entitlements record indicating that he or she is covered by the payer associated with that program billing group. Documented services that meet the documentation requirements entered for that billing type are also required.
![]() NOTE: Invoices are generated for program billing groups, not individual programs. For more information about program billing groups, click here.
NOTE: Invoices are generated for program billing groups, not individual programs. For more information about program billing groups, click here.
To generate a batch of invoices, complete the following steps:
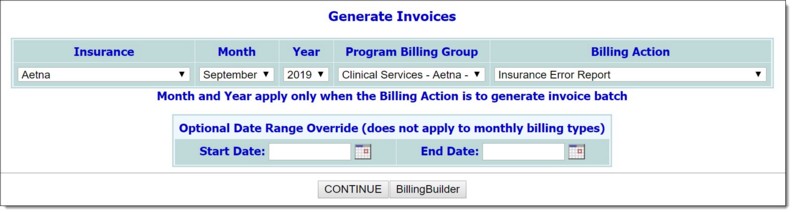
![]() TIP: A month and year must be selected for "monthly" billing types. For "per diem" or "fee for service" billing types, the optional date range override may be used to generate invoices for a period shorter than one month. See step 8 for further instructions.
TIP: A month and year must be selected for "monthly" billing types. For "per diem" or "fee for service" billing types, the optional date range override may be used to generate invoices for a period shorter than one month. See step 8 for further instructions.
![]() Insurance Error Report - Displays all clients who are missing important information needed to create an invoice (such as diagnosis, insurance ID, etc.)..
Insurance Error Report - Displays all clients who are missing important information needed to create an invoice (such as diagnosis, insurance ID, etc.)..
![]() Generate Invoice Batch - Creates newly billed invoices (primary invoices) if the following is true; otherwise, a secondary or tertiary invoice could be generated:
Generate Invoice Batch - Creates newly billed invoices (primary invoices) if the following is true; otherwise, a secondary or tertiary invoice could be generated:
The payer is primary and there is not a future record (re-bill) for the consumer for the date of service.
If this is not the case and one of the following are true, then a non-primary invoice could be created using this billing action:
The payer is secondary and there are no future records (re-bill) for the consumer on the date of service/procedure, and there is remittance information for the primary payer for the same date of service/procedure.
- OR -
The primary does not have a billable procedure with the same HCPCS/CPT code.
![]() Generate Bulk Manual Batch - Provides the ability to create a batch of invoices manually. In order to use this option, the billing type associated with the program billing group selected when creating an invoice batch must have the "No Billing Rules Entered in AWARDS" option checked.
Generate Bulk Manual Batch - Provides the ability to create a batch of invoices manually. In order to use this option, the billing type associated with the program billing group selected when creating an invoice batch must have the "No Billing Rules Entered in AWARDS" option checked.
![]() Generate Previously Ineligible Batch - Creates invoices for previously ineligible records (for Medicaid billing only).
Generate Previously Ineligible Batch - Creates invoices for previously ineligible records (for Medicaid billing only).
![]() Generate Claim Denials Re-Billing Batch - Creates invoices for previously denied invoices (marked as re-bill in a worksheet).
Generate Claim Denials Re-Billing Batch - Creates invoices for previously denied invoices (marked as re-bill in a worksheet).
![]() Generate COB Remainders Re-Billing Batch - Creates invoices for invoices where a remainder was assigned in a worksheet.
Generate COB Remainders Re-Billing Batch - Creates invoices for invoices where a remainder was assigned in a worksheet.
![]() Generate Denials and Remainders Re-Billing Batch - Creates invoices for both previously denied invoices (marked as re-bill) in a worksheet and invoices where a remainder was assigned in a worksheet.
Generate Denials and Remainders Re-Billing Batch - Creates invoices for both previously denied invoices (marked as re-bill) in a worksheet and invoices where a remainder was assigned in a worksheet.
![]() Generate All Futures Batch - Creates invoices for Ineligible, Denied, and Remainder Assigned invoices.
Generate All Futures Batch - Creates invoices for Ineligible, Denied, and Remainder Assigned invoices.
![]() Verify Invoice - Displays reasons why an invoice was not created for a client (for example, service documentation did not match the procedure requirements).
Verify Invoice - Displays reasons why an invoice was not created for a client (for example, service documentation did not match the procedure requirements).
![]() Generate Empty Batch - Provides the ability to create a batch of invoices manually, with no required settings.
Generate Empty Batch - Provides the ability to create a batch of invoices manually, with no required settings.
The process of generating invoices is now complete.
![]() TIP: To view the batch details, or to update or delete the generated batch of invoices from this page, click the View, Update, or Delete button as appropriate. These features are explained in detail here.
TIP: To view the batch details, or to update or delete the generated batch of invoices from this page, click the View, Update, or Delete button as appropriate. These features are explained in detail here.
https://demodb.footholdtechnology.com/help/?11432