|   |
|   |
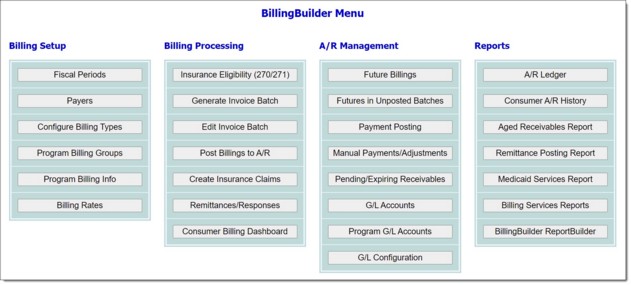
The Future Billings feature is used to generate a list of invoices that were either marked for re-billing, or where the client was ineligible when the insurance company was initially billed. To do so, complete the following steps:

![]() All Re-Billing for Denials and Remainders - Displays all records that were created from a re-bill invoice, and records created from a remainder being assigned.
All Re-Billing for Denials and Remainders - Displays all records that were created from a re-bill invoice, and records created from a remainder being assigned.
![]() Claim Denials to be Re-Billed - Displays only invoices that have been marked as "Re-bill" within a posted worksheet.
Claim Denials to be Re-Billed - Displays only invoices that have been marked as "Re-bill" within a posted worksheet.
![]() Claim Remainders Assigned to COB Re-Billing - Displays records created from a remainder being assigned.
Claim Remainders Assigned to COB Re-Billing - Displays records created from a remainder being assigned.
![]() Ineligible When Invoices Were Generated - Displays all clients who did not have a Medicaid entitlement present when the payer was originally billed.
Ineligible When Invoices Were Generated - Displays all clients who did not have a Medicaid entitlement present when the payer was originally billed.
![]() NOTE: This option only applies to Medicaid entitlements and hard-coded billing types (PROS, ACT, CR, DD, etc.).
NOTE: This option only applies to Medicaid entitlements and hard-coded billing types (PROS, ACT, CR, DD, etc.).
![]() Include All - Displays all invoices.
Include All - Displays all invoices.
![]() # - Displays a numerical listing for all invoices that appear on the report.
# - Displays a numerical listing for all invoices that appear on the report.
![]() Delete? - Check off this option to void the original invoice and void the open receivable. If a future invoice was created in error, it can be removed using this option. Click CONTINUE to proceed with the deletions.
Delete? - Check off this option to void the original invoice and void the open receivable. If a future invoice was created in error, it can be removed using this option. Click CONTINUE to proceed with the deletions.
![]() Program - Displays the program associated with the original invoice.
Program - Displays the program associated with the original invoice.
![]() Invoice Date - Displays the date on which the original invoice was created.
Invoice Date - Displays the date on which the original invoice was created.
![]() Consumer - Displays the consumer associated with the future billing line item.
Consumer - Displays the consumer associated with the future billing line item.
![]() Reason - Displays the reason for the future billing entry: previously denied, remainder assigned, payer, and worksheet where the future record was created.
Reason - Displays the reason for the future billing entry: previously denied, remainder assigned, payer, and worksheet where the future record was created.
![]() Original Amount - Displays the amount associated with the initial invoice. The amount associated with the future record displays in parentheses and may or may not match the original amount.
Original Amount - Displays the amount associated with the initial invoice. The amount associated with the future record displays in parentheses and may or may not match the original amount.
![]() Original Invoice - Displays the Invoice ID and Batch ID associated with the initial invoice created.
Original Invoice - Displays the Invoice ID and Batch ID associated with the initial invoice created.
![]() Insurance - Displays the payer associated with the future record. This column of data is only shown when "All Payers" was selected from the Insurance drop-down on the previous page.
Insurance - Displays the payer associated with the future record. This column of data is only shown when "All Payers" was selected from the Insurance drop-down on the previous page.
The process of viewing a future billings report is now complete.
https://demodb.footholdtechnology.com/help/?11823